SHHA Summit: ‘the imperative is promoting healthy ageing’
Some megatrends are affecting the future of care for older people in a fast-ageing society and both the public and private sectors should be aware of them, delegates heard at the SHHA Summit, which took place in Brussels this week and was hosted by Deloitte.

“The biggest megatrend is ageing, so fostering healthy ageing is an imperative now”, said Karolin Killmeier, Policy Analyst in the OECD´s Health Division, Directorate for Employment, Labour & Social Affairs. “The share of older people is increasing and so is the severity of their needs. The number of people with severe needs will keep increasing beyond 2050.”
The data are clear: 3 out of 10 people will be over 65 by 2050 and one out of four older people already needs care today, but by 2050 there will be a 30% increase – meaning two out of five people will have severe care needs.
“This means that public care expenditure must increase by 2.6% a year on average just to maintain the current level of support”, said Killmeier. “What is needed is to fund better, target better and spend better.”
Better funding means diversifying funding sources going beyond income tax revenues and developing innovative schemes. Targeting better means giving a greater share of funding to those who have more severe needs and lower income. Spending better means investing more in prevention, rehabilitation and technology to make sure people live longer in better health, and promoting better health care models.
“There are some good examples already, like the Nordic countries doing preventive home visits or Poland’s primary care centres pooling different professions under one roof with specific expertise on over-75s”, said Killmeier. “Ireland has specific care pathways for older people and Japan has community-based integrated care.”
One megatrend that gives reasons for optimism is the promising technological advances that will change what has traditionally been a labour-intensive sector.
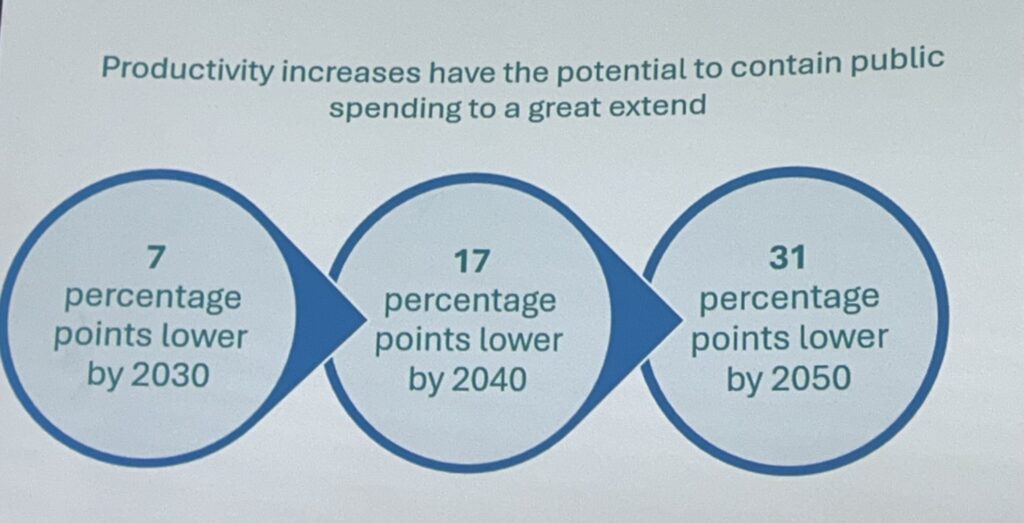
“Productivity increases have the potential to contain public spending to a great extent”, she said. “It is a bold prediction, but we foresee a 7% reduction by 2030, rising to 17% by 2040 and 31% by 2050.”
Another megatrend is the clear preference for home-based care in all OECD countries, even if the vast majority of the money spent goes on residential care, up to 90% in some places. Some countries are realising this and changing their approach: Australia, for example, is reforming its support at home scheme, adapting homes and helping people remain active in their communities.
“We need innovative residential building solutions to make communities more age-friendly”, said Killmeier. “Regulations should be adjusted to fund new forms of living for older people, supporting independence and autonomy, promoting social inclusion, respecting people´s lifestyle choices and allowing them to remain active and healthy for as long as possible.”
Significantly, people are not only aware of the problem but they are willing to do something about it. According to OECD surveys, 65% of respondents are concerned about accessing good quality long-term care and that percentage rises to over 80% in some countries like Spain, Greece and Portugal. Many people say they are willing to pay 2% more in taxes to fund better public long-term care.



